- 3.11.29 Health Coverage Tax Credit (HCTC) Enrollment Processing
- 3.11.29.1 Program Scope and Objectives
- 3.11.29.1.1 Background
- 3.11.29.1.2 Authority
- 3.11.29.1.3 Roles and Responsibilities
- 3.11.29.1.4 Program Reviews
- 3.11.29.1.5 Program Controls
- 3.11.29.1.6 IDRS Notice Issuance
- 3.11.29.1.7 Acronyms
- 3.11.29.2 Deviations from the IRM
- 3.11.29.3 Reporting Time - Organization Function Program (OFP)
- 3.11.29.4 HCTC Program General Information
- 3.11.29.5 Access to the HCTC Database
- 3.11.29.6 Form 13441-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update
- 3.11.29.7 Batching Form 13441-A
- 3.11.29.8 Initial Review of Form 13441-A
- 3.11.29.9 Inputting Form 13441-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update, Into the Database
- 3.11.29.9.1 Inputting Form 13441-A, Part 1: Your General Information
- 3.11.29.9.1.1 Determining Eligibility
- 3.11.29.9.2 Inputting Form 13441-A, Part 2: Confirm Your Eligibility
- 3.11.29.9.3 Inputting Form 13441-A, Part 3: Family Member Information
- 3.11.29.9.4 Inputting Form 13441-A, Part 4: Health Plan Information
- 3.11.29.9.5 Inputting Form 13441-A, Part 5: Account Accessibility
- 3.11.29.9.6 Inputting Form 13441-A, Part 6: Form Completion
- 3.11.29.9.1 Inputting Form 13441-A, Part 1: Your General Information
- 3.11.29.10 Setting the Status of the Application
- 3.11.29.11 Systemically Generated Statuses of the Application
- 3.11.29.12 Releasing / Filing Forms 13441-A, Batches
- 3.11.29.13 Correspondence
- 3.11.29.13.1 Letter 3772, End of Program Letter
- 3.11.29.13.2 Letter 4510, HCTC Reimbursement Request - Denial
- 3.11.29.13.3 Letter 4511, HCTC Reimbursement Request - Insufficient Documentation
- 3.11.29.13.4 Letter 4540, HCTC Candidate Eligibility Denial
- 3.11.29.13.5 Letter 4545, HCTC Enrollment Letter
- 3.11.29.13.6 Letter 5758, Health Coverage Tax Credit Enrollment in Process
- 3.11.29.13.7 Letter 5945, HCTC Reimbursement Approval
- 3.11.29.13.8 Letter 5974, Annual HCTC Vendor Renewal Notification
- 3.11.29.13.9 Letter 6009, Refund of HCTC Payments
- 3.11.29.13.10 Letter 6011, Return of HCTC Funds
- 3.11.29.14 Form 4442, Participant Correspondence, and US Bank Correspondence
- 3.11.29.15 Qualifying Family Member Participant (QFMP)
- 3.11.29.16 Processing Form 14095, The Health Coverage Tax Credit (HCTC) Reimbursement Request Form
- 3.11.29.16.1 Form 14095, Part 2: Determine Eligibility and Request Reimbursement
- 3.11.29.16.2 Form 14095, Part 3: Gathering Supporting Documents
- 3.11.29.16.3 Form 14095, Part 4: Sign and Date This Form
- 3.11.29.17 Replies to Form 14095, The Heath Coverage Tax Credit (HCTC) Reimbursement Request Form
- 3.11.29.18 SF-1034, Public Voucher for Purchases and Services other than Personal, Monthly Payment Reconciliation
- 3.11.29.18.1 Completing SF-1034
- 3.11.29.19 Form 8885, Health Coverage Tax Credit
- 3.11.29.20 Form 3881-A, ACH Vendor / Miscellaneous Payment Enrollment – HCTC
- 3.11.29.20.1 Submitting Form 3881-A
- 3.11.29.20.2 Recertifying with Form 3881-A
- 3.11.29.21 Payment Submission / Lockbox / Daily Mail-Out Package
- 3.11.29.22 Insufficient Funds Notification
- 3.11.29.23 Rejected Payments by Vendors
- 3.11.29.24 Operations Assistance Request (OARs)
- 3.11.29.25 Record Retention Requirements
- 3.11.29.26 Daily Reports
- 3.11.29.27 Weekly Reports
- Exhibit 3.11.29-1 Letter 3772 - End of Program Letter
- Exhibit 3.11.29-2 Letter 4510 - HCTC Reimbursement Request Denial
- Exhibit 3.11.29-3 Letter 4511 - HCTC Reimbursement Request - Insufficient Documentation
- Exhibit 3.11.29-4 Letter 4540 - HCTC Notice of Ineligibility
- Exhibit 3.11.29-5 Letter 4545 - HCTC Enrollment Letter
- Exhibit 3.11.29-6 Letter 5758 - Health Coverage Tax Credit Enrollment in Process
- Exhibit 3.11.29-7 Letter 5945 - HCTC Reimbursement Approval
- Exhibit 3.11.29-8 Letter 5974 - Annual HCTC Vendor Renewal Notification
- Exhibit 3.11.29-9 Letter 6009 - Refund of HCTC Payments
- Exhibit 3.11.29-10 Letter 6011 - Return of HCTC Funds
- 3.11.29.1 Program Scope and Objectives
Part 3. Submission Processing
Chapter 11. Returns and Documents Analysis
Section 29. Health Coverage Tax Credit (HCTC) Enrollment Processing
3.11.29 Health Coverage Tax Credit (HCTC) Enrollment Processing
Manual Transmittal
October 20, 2021
Purpose
(1) This transmits revised IRM 3.11.29, Health Coverage Tax Credit (HCTC) Enrollment Processing.
Material Changes
(1) IRM 3.11.29.1.1(1) Added new HCTC extension legislation for 2021. IPU 21U0120 issued 01-21-2021
(2) IRM 3.11.29.5 Replaced Online 5081 with BEARS due to Online 5081 no longer used for requesting access.
(3) IRM 3.11.29.7 (Note) Updated checkbox number due to Form 13441-A revision. IPU 21U0120 issued 01-21-2021
(4) IRM 3.11.29.8(9) chart, Added instructions to notify P&A if remittance is discovered in HCTC documentation, allowing further research to be performed. IPU 20U1243 issued 11-17-2020
(5) IRM 3.11.29.9(4) second row in chart, Removed duplicate IRM reference. IPU 21U0749 issued 05-19-2021
(6) IRM 3.11.29.9(4) second row in chart, Replaced Letter 4541 with Letter 4540, with appropriate correspondence fill-in, due to Letter 4541 no longer being used. IPU 21U0741 issued 05-18-2021
(7) IRM 3.11.29.9.1.1(7) (c) Fixed grammatical error. IPU 21U0749 issued 05-19-2021
(8) IRM 3.11.29.9.2(5) Added instruction to edit QFMP dates due to 24-month eligibility legislation. IPU 21U0439 issued 03-19-2021
(9) IRM 3.11.29.9.4(3) Added re-enrollments to the vendor verification requirement. IPU 21U0120 issued 01-21-2021
(10) IRM 3.11.29.9.4(3)(b) Removed P&A and replaced with HQ, since HQ obtains required fields from vendors. IPU 21U0120 issued 01-21-2021
(11) IRM 3.11.29.9.4(5) Updated paragraph number due to Letter 4540 revision. IPU 21U0741 issued 05-18-2021
(12) IRM 3.11.29.9.4(11) Added instruction to remove COBRA dates when a participant indicates that they are changing to a non-COBRA plan. IPU 21U0120 issued 01-21-2021
(13) IRM 3.11.29.9.6(2) (b) Replaced Letter 4541 with Letter 4540. IPU 21U0741 issued 05-18-2021
(14) IRM 3.11.29.10 (Note) Added instruction to notify P&A when a participant is moved out of enrolled status, allowing further research to be performed. IPU 20U1243 issued 11-17-2020
(15) IRM 3.11.29.10 chart, Clarified status selection when HPA is not enrolled or qualified. IPU 21U0346 issued 03-05-2021
(16) IRM 3.11.29.10(2) chart, Removed Letter 4541 references and updated title and paragraphs for Letter 4540. IPU 21U0741 issued 05-18-2021
(17) IRM 3.11.29.10(2) (Second Note) Deleted note since Letter 4541 is no longer used. IPU 21U0741 issued 05-18-2021
(18) IRM 3.11.29.12(7) Added additional year for files storage due to the one-year extension. IPU 21U0120 issued 01-21-2021
(19) IRM 3.11.29.13 chart, Removed Letter 4541 reference and updated Letter 4540 title and purpose. IPU 21U0741 issued 05-18-2021
(20) IRM 3.11.29.13(12) (Note) Deleted references to faxes due to US Bank now only accepting emails. IPU 21U0346 issued 03-05-2021
(21) IRM 3.11.29.13.1(3) Updated status due to “Cancelled-Permanent Ineligibility” no longer in use. IPU 21U0439 issued 03-19-2021
(22) IRM 3.11.29.13.4 Updated title for Letter 4540. IPU 21U0741 issued 05-18-2021
(23) IRM 3.11.29.13.4(1) Updated title and purpose for Letter 4540 due to the merging of Letter 4541 onto Letter 4540. IPU 21U0741 issued 05-18-2021
(24) IRM 3.11.29.13.4(3) (4) Removed Letter 4541 references and instructions. IPU 21U0741 issued 05-18-2021
(25) IRM 3.11.29.13.4(6) Updated number of selectable paragraphs on Letter 4540 due to revision. IPU 21U0741 issued 05-18-2021
(26) IRM 3.11.29.13.4(6) (e) Updated paragraphs due to Letter 4540 revision. IPU 21U0741 issued 05-18-2021
(27) IRM 3.11.29.13.4(6) (Reminder) Removed due to Letter 4541 no longer being used. IPU 21U0741 issued 05-18-2021
(28) IRM 3.11.29.13.4(6) Updated titles of paragraphs throughout, Letter 4540, due to the merging of Letter 4541 onto Letter 4540. IPU 21U0741 issued 05-18-2021
(29) IRM 3.11.29.13.4(9) Updated Enclosure title due to Letter 4540 revision. IPU 21U0741 issued 05-18-2021
(30) IRM 3.11.29.13.4(10) Added instruction for incomplete replies after 45-day suspense period and clarified which paragraphs should be selected on Letter 4540 when corresponding a second time. IPU 20U0913 issued 08-14-2020
(31) IRM 3.11.29.13.5 Deleted section due to Letter 4541 no longer being used. IPU 21U0741 issued 05-18-2021
(32) IRM 3.11.29.13.5(9) Added instruction for incomplete replies after 45-day suspense period and clarified which paragraphs should be selected on Letter 4540 when corresponding a second time. IPU 20U1012 issued 09-16-2020
(33) IRM 3.11.29.13.10(2) Changed Beckley Finance Center to IRS Beckley Office.
(34) IRM 3.11.29.14(5) (d) Added instruction to route substitute Form 4442 to QR. IPU 21U0976 issued 07-23-2021
(35) IRM 3.11.29.14(5) (d) (Note) Fixed grammatical error. IPU 21U0741 issued 05-18-2021
(36) IRM 3.11.29.15(7) chart, Corrected QFM qualifying date, due to Medicare eligibility, since both Medicare recipient and qualifying family member are eligible the entire birth month in which the Medicare recipient turns 65. IPU 21U0267 issued 02-16-2021
(37) IRM 3.11.29.15(8) (b)(c) Added form number to clarify where information is pulled from. IPU 21U0741 issued 05-18-2021
(38) IRM 3.11.29.15(8) (f) Added additional instruction for when an eligible participant does not have an established PIN. IPU 21U0741 issued 05-18-2021
(39) IRM 3.11.29.15(8) (g) Added instruction to elevate to P&A when eligible recipient is included in Part 3, Form 13441-A to allow for additional research. IPU 21U0439 issued 03-19-2021
(40) IRM 3.11.29.15(8) (j) Added instruction to enter eligible recipient’s name and PIN on QFMP’s record in order to record source of eligibility. IPU 21U0439 issued 03-19-2021
(41) IRM 3.11.29.15(8) (j) Removed duplicate instruction already included in (8)(f). IPU 21U0741 issued 05-18-2021
(42) IRM 3.11.29.15(8) (k) Added instruction to enter QFMP’s name and PIN on eligible recipient’s record in order to record QFMP’s source of eligibility. IPU 21U0439 issued 03-19-2021
(43) IRM 3.11.29.16(3) (f)(g) Reversed bullets to correct order of processing steps. IPU 21U0741 issued 05-18-2021
(44) IRM 3.11.29.16(7) Added instruction for P&A to send HQ confirmation of Form 14095 correspondence.
(45) IRM 3.11.29.16.3 (c) Removed suspense instruction due to Form 14095 being processed by P&A and not by Tax Examiners. IPU 20U0913 issued 08-14-2020
(46) IRM 3.11.29.18 Clarified Form 1034 reimbursement process. IPU 21U0976 issued 07-23-2021
(47) IRM 3.11.29.18 Replaced individuals with participants for consistency. IPU 21U0976 issued 07-23-2021
(48) IRM 3.11.29.18(4) (b) Replaced individuals with participants for consistency. IPU 21U0976 issued 07-23-2021
(49) IRM 3.11.29.18(5) Added instruction for P&A to send HQ confirmation of Form 1034 correspondence. IPU 21U0976 issued 07-23-2021
(50) IRM 3.11.29.18(6) Removed ET instructions due to HQ handling vendor 1034’s. IPU 21U0556 issued 04-09-2021
(51) IRM 3.11.29.18(6) Replaced reimbursement with disbursement. IPU 21U0976 issued 07-23-2021
(52) IRM 3.11.29.18(7) Updated where 1034’s are entered in the HCTC Database. IPU 21U0741 issued 05-18-2021
(53) IRM 3.11.29.18(7)(b) Updated back-up certifying officer for vendor’s SF-1034 due to operational staffing changes. IPU 20U1012 issued 09-16-2020
(54) IRM 3.11.29.18(7)(b) Updated back-up certifying officer for vendor’s SF-1034 due to operational staffing changes. IPU 21U0439 issued 03-19-2021
(55) IRM 3.11.29.18.1(1) Replaced reimbursement with disbursement. IPU 21U0976 issued 07-23-2021
(56) IRM 3.11.29.18.1(1) (2nd bullet) Updated 1034 completion instructions due to the Enrollment Team no longer preparing. IPU 21U0741 issued 05-18-2021
(57) IRM 3.11.29.20.2 (a) Deleted instruction due to Beckley no longer sending monthly notifications. IPU 21U0741 issued 05-18-2021
(58) IRM 3.11.29.21 Deleted references to faxes due to US Bank now only accepting emails. IPU 21U0346 issued 03-05-2021
(59) IRM 3.11.29.21(9)(a) Deleted fax number and added new email address. IPU 21U0346 issued 03-05-2021
(60) IRM 3.11.29.22(1) Replaced Lockbox with CFO due to CFO sending insufficient funds notifications. IPU 21U0741 issued 05-18-2021
(61) IRM 3.11.29.22(2) Removed P&A due to HQ working insufficient funds. IPU 21U0741 issued 05-18-2021
(62) IRM 3.11.29.23 Changed section title to clarify type of rejected payment. IPU 21U0741 issued 05-18-2021
(63) IRM 3.11.29.23(1) Removed incorrect instruction for this section. IPU 21U0741 issued 05-18-2021
(64) IRM 3.11.29.23(2) Removed P&A due to HQ working rejected vendor payments. IPU 21U0741 issued 05-18-2021
(65) IRM 3.11.29.23(3) Added CFO instruction for sending rejected vendor payment notifications. IPU 21U0741 issued 05-18-2021
(66) IRM 3.11.29.25(1) Added additional year for files storage due to the one-year extension. IPU 21U0141 issued 01-25-2021
(67) IRM 3.11.29.27(4) Changed Beckley Finance Center to IRS Beckley Office.
(68) Various editorial changes made throughout to update spelling, grammar, IRM references, etc.
(69) Exhibit 3.11.29-5 Deleted due to Letter 4541 no longer being used. IPU 21U0741 issued 05-18-2021
Effect on Other Documents
IRM 3.11.29, Health Coverage Tax Credit (HCTC) Enrollment Processing dated June 24, 2020, is superseded. The following IRM Procedural Updates (IPUs) issued August 14, 2020 through July 23, 2021, have been incorporated into this IRM: 20U0913, 20U1012, 20U1243, 21U0120, 21U0141, 21U0267, 21U0346, 21U0439, 21U0556, 21U0741, 21U0749, and 21U0976.Audience
Employees in the Austin Submission Processing Center and Customer Service Representatives in Accounts Management.Effective Date
(01-01-2022)
James L. Fish
Director, Submission Processing
Wage and Investment Division
-
Purpose: This IRM provides guidance on the Health Coverage Tax Credit (HCTC).The Enrollment Team evaluates eligibility for the monthly advance payment, enters information from Form 13441-A into a database, authorizes payment of the credit, and sets up approved HCTC vendors for ACH payments.
-
Audience: The HCTC Enrollment Team, in Austin, is the primary user of this IRM.
-
Policy Owner: The Director of Submission Processing
-
Program Owner: Wage and Investment (W&I) Submission Processing
-
Primary Stakeholders: The HCTC Enrollment Team in Austin
-
Program Goals: The information contained in this IRM provides the HCTC Enrollment Team instructions to evaluate eligibility for the advance monthly payments of the HCTC.
-
The Health Coverage Tax Credit (HCTC), authorized in the Trade Adjustment Assistance Reform Act of 2002, first became effective for coverage months beginning after August 6, 2002. The HCTC later expired for coverage months after 2013. But the Trade Adjustment Assistance Reauthorization Act of 2015 restored the HCTC retroactively for 2014 coverage, erasing the hiatus in its duration, and extended it for coverage through the end of 2019. On December 20, 2019, Congress passed H.R. 1865, Further Consolidated Appropriations Act, 2020, which included an extension of the HCTC program through December 31, 2020. HCTC Legislation was extended again, through December 31, 2021, under The Taxpayer Certainty and Disaster Tax Relief Act of 2020, Section 134.
-
The HCTC subsidizes most of the cost of qualified health insurance for eligible individuals and their eligible family members. The credit pays 72.5% of the insurance premiums while the participant enrolled in the program pays 27.5% of the premiums.
-
Eligibility for the HCTC is restricted to two groups of individuals:
-
Individuals who are eligible for benefits under the program Trade Adjustment Assistance (TAA) because of a qualifying job loss and receive benefits through the Trade Readjustment Allowance (TRA), Reemployment Trade Adjustment Assistance (RTAA), or Alternative Trade Adjustment Assistance (ATAA)
-
Individuals who are between 55 and 64 years old, whose defined benefit pension plans were taken over by the Pension Benefit Guaranty Corporation (PBGC), and are not enrolled in Medicare
-
-
Individuals eligible for the HCTC are allowed the tax credit only if:
-
they aren’t enrolled in certain government-or employer-subsidized health coverage (Medicaid, for instance).
-
they aren’t eligible for other specified coverage (Medicare Part A or TRICARE) and
-
they cannot be claimed as a dependent on another person’s federal income tax return.
-
-
To apply for the HCTC, applicants submit Form 13441-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update, and the required supporting documents to IRS, Mail Stop 6098 AUSC, Austin, TX 78741.
-
Authority for these procedures is found in Internal Revenue Code IRC 7527.
-
All Policy Statements for Submission Processing are contained in IRM 1.2.1.4, Policy Statements for Submission Processing Activities.
-
The Director of Submission Processing oversees policy and guidance for employees of the Austin Submission Processing Center and ensuring consistent application of policies and procedures to effect tax administration while protecting taxpayers’ rights.
-
The Submission Processing Field Director, reports to the Director Submission Processing, and manages the delivery of policy and guidance that impacts the HCTC Advance Monthly Payment process.
-
The Operation Manager implements policy and guidance that impacts the HCTC Advance Monthly Payment process.
-
All employees must perform their professional responsibilities in a way that supports the IRS Mission in order to provide top quality service and to apply the law with integrity and fairness to all.
-
The HCTC program is an unmeasured program for production. However, due to the nature of the program, all applications, changes, reimbursement requests, and correspondence are 100% quality reviewed.
-
Instructions issued by the P&A Staff are reviewed by Planning & Analysis (P&A) and/or Headquarters (HQ). The Quality Review team should ensure that the instructions are correctly followed but are not responsible for reviewing the content of those instructions.
-
IRS will implement access control measures that will provide protection from unauthorized alteration, loss, unavailability, or disclosure of information. Access controls will follow the principle of access enforcement, least privilege, separation of duties, system-use notifications, session locks, and session lock-control enhancements as defined in IRM 10.8.1, Information Technology (IT) Security, Policy and Guidance.
-
While working assigned cases, Submission Processing employees may come across some accounts that are blocked on IDRS and can be identified by an IDRS security violation message, "Unauthorized Access to this Account" . Forward the case to your manager. Managers will notify the local Planning & Analysis Staff who will scan the case and send encrypted information to the ≡ ≡ ≡ ≡ ≡ ≡ mailbox to request access to the account. Managers will retain the case in a file awaiting access (can take up to 5 business days). Once notified access has been granted, the documents can be worked following applicable procedures.
-
Following are commonly used acronyms:
Acronym Meaning ATAA Alternative Trade Adjustment Assistance COBRA Consolidated Omnibus Budget Reconciliation Act DOL Department of Labor DPO Document Perfection Operation DSRA-BT Delphi Salaried Retirees Association Benefit Trust HCTC Health Coverage Tax Credit HPA Health Plan Administrator IDRS Integrated Data Retrieval System P&A Planning and Analysis PBGC Pension Benefit Guaranty Corporation PIN Participant Identification Number QFM Qualifying Family Member QFMP Qualifying Family Member Participant RCO Receipt Control Operation RTAA Reemployment Trade Adjustment Assistance SWA State Workforce Agency TAA Trade Adjustment Assistance TPA Third Party Administrator TRA Trade Readjustment Allowance
-
Service Center Directors, Headquarter Branch Chiefs, and Headquarter Analysts do not have the authority to approve deviations from IRM procedures. Any request for an exception or deviation to an IRM procedure must be elevated through appropriate channels for executive approval. This will ensure that other functional areas are not adversely affected by the changes and that it does not result in disparate treatment of taxpayers.
-
See guidelines in IRM 1.11.2, Internal Revenue Manual (IRM) Process. Request for an IRM deviation must be submitted in writing and signed by the Field Director, following instructions from IRM 1.11.2.2.4. Any disclosure issues will be coordinated by the Program Owner. No deviations can begin until they are reviewed by the Program Owner and approved at the Executive Level. All requests must be submitted to the Submission Processing Headquarters IRM Coordinator.
-
Report all time spent in processing or handling HCTC forms with the organization, program, and function codes (OFP) below.
Function/Program WP&C Title Application Type 390-84310 F14095 Original Form 14095 390-84311 14095COR F14095 correspondence 390-84312 14095RPL F14095 reply to correspondence 390-84313 14095NOR F14095 without a reply to correspondence 390-84330 HCTC New Form 13441-A applications 390-84331 HCTCUPDT Updated F13441-A applications 390-84332 HCTC4442 Inquiries with Form 4442 or from US Bank 390-84333 HCTCCORR Forms with correspondence (suspense) 390-84334 HCTCRPLY Forms with a reply to correspondence 390-84335 HCTCNORP Forms without a reply to correspondence 770-84310 F14095 Clerical - Form 14095 770-84330 HCTC Clerical - Form 13441-A
-
All forms, correspondence, or other participant documentation must be processed following the general guidelines below.
-
Any necessary editing should be done in erasable red ink.
-
TE stamp each document processed.
-
Verify the received date is present and legible. If not, edit the first available date from the list below in the "Rcvd MMDDYY" format.
-
Latest postmark on the envelope, the latest date from a designated private delivery service, or electronic transmission date (date of fax or e-mail)
-
Service Center Automated Processing System (SCAMPS) digital date
-
Participant’s latest signature date
-
Today’s date
-
-
All forms, correspondence, and documentation should be stapled to the back of Form 13441-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update, in Received Date order with the oldest (Original) Form 13441-A stapled to the top. If an updated Form 13441-A is submitted, then any prior Form 13441-A should be "X’d."
-
If any information on HCTC forms is "X’d," crossed out, or lined through, either pre-printed or manually, it should be considered invalid.
-
If a record is entered in error, refer the application to the HCTC Coordinator.
-
Never obliterate, alter or erase the original entry on a document when deleting or correcting an entry. Circle out invalid information, making sure the original entry remains legible.
-
When detaching documentation, edit an action trail:
-
On the application, which includes:
- Item detached
- Current Date (MMDDYY)
- Participant Identification Number -
On the detached document, which includes:
- Form the document was detached from
- Current Date (MMDDYY)
- Participant’s Name
- Participant Identification Number
-
-
Comments must be entered into the HCTC database for any correspondence, inquiry, or action to participants account. Comments must be specific and include the nature of the action taken.
-
If a change to the participant’s database entry changes the "Last Modified" date, all entries in the database must be verified for accuracy. Ensure all information in the database is supported by documentation in the applicant’s file.
-
Anytime a record is updated in the database, see IRM 3.11.29.12, Setting the Status of the Application.
-
The participant’s file should be present when processing updates which affect the Last Modified date, to allow the required research to be performed.
Exception:
End-of-year attestation spreadsheets are received from the vendor and allow for rate changes only; TE’s are not required to review all entries. The participant's file is not required to be present if submitted per this exception, however the Forms 4442 will need to be added to each participant's file no later than one week following the update.
-
Forms and correspondence received by the HCTC Enrollment Team are to be processed or routed within 5 business days from the date received by the Enrollment Team.
Exception:
Some forms and correspondence received for processing by the HCTC Enrollment Team are not effective until a future date. Review any item effective on a future date for correspondence conditions and correspond if necessary. Once the file is processable, suspend until the 20th day of the month prior to the effective date.
-
If the participant’s Participant Identification Number begins with 100006, they are an interim participant who was added to the program before the current database was available. When processing a change to an interim participant’s database entry, review all blank fields (both required and non-required).
-
In some cases, it is necessary to elevate a question or issue to P&A and/or HQ for resolution. Once elevated, suspend the document until a response is received but not longer than 10 business days. Once a response is received, the document should be rebatched and processed following normal timeliness guidelines.
-
Some database fields have character restrictions which prevent information from being entered as provided/perfected. If one or more characters are invalid for the field, enter the information while omitting the special character.
-
For Tax Examiners to process, edit, and review HCTC forms, they must request access to the HCTC Database through the Business Entitlement Access Request System (BEARS).
-
Roles are granted based on job duties as follows:
Role BEARS Application Name and Group Clerk PROD USER HCTC CLERK DR USER HCTC CLERK Examiner PROD USER HCTC TAX EXAMINER Reviewer PROD USER HCTC QUALITY REVIEWER DR USER HCTC QUALITY REVIEWER Customer Service PROD USER HCTC READ ONLY DR USER HCTC READ ONLY Admin PROD USER HCTC ADMIN (HEALTH COVERAGE TAX CREDIT-HCTC) Reports PROD USER HCTC REPORTS (HEALTH COVERAGE TAX CREDIT-HCTC) -
A warning that the database is for authorized use only appears when accessing the database. Users must accept the terms of use to open the database.
-
Form 13441-A , Health Coverage Tax Credit (HCTC) Monthly Registration and Update, is processed in two operations in Austin Submission Processing: Receipt & Control (RCO) and Document Perfection (DPO).
-
In RCO, clerks receive, extract, and Receive Date stamp Form13441-A. RCO then routes Form 13441-A to DPO’s Entity Enrollment Team at AUSC Stop 6098 at the Austin Service Center.
-
In DPO, clerks in the Entity Enrollment Team batch Form 13441-A. Tax Examiners screen enrollment Forms 13441-A for completeness and to determine any need for correspondence. They will accept or correspond for the correction of defects.
-
-
Batching Form 13441-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update, occurs in the Entity Enrollment Team.
-
Separate new Forms 13441-A from updated Forms 13441-A. Batch new and old separately.
-
Follow instructions in IRM 3.10.5.6.4, Image Control Team (ICT) Batch Creation Screen, for creating batches in the BBTS system.
-
Batch Forms 13441-A by the date the form was received in Entity, in groups of 25. Each form in the batch must have been received on the same date.
-
Print batch transmittals and associate the transmittals with their batches.
-
Stage batches by the date received in the designated work area.
-
Verify the applicant signed the form in Part 6 prior to updating the database. See IRM 3.11.29.9.6, Inputting Form 13441-A Part 6: Form Completion.
-
Edit a Received Date on the first page of Form 13441-A, if missing. See IRM 3.11.29.4, HCTC Program General Information.
-
Stamp your Tax Examiner number in the upper left of the first page of Form 13441-A.
-
Verify Form 13441-A is batched correctly. If the form is in the wrong batch, remove the form and have the clerk re-batch.
-
New enrollments should be reviewed for QFMP status, see IRM 3.11.29.15, Qualifying Family Member Participant (QFMP).
-
A health insurance bill (or other document(s) which meet the criteria below) dated within the last sixty days must be present when enrolling or if updating their vendor and/or premium information. If information below is not available, see IRM 3.11.29.13, Correspondence:
-
Name of applicant (may be the policy holder or a covered individual on policy. See IRM 3.11.29.9, Inputting Form 13441-A.)
-
Dates of coverage
-
Amount of monthly premium
-
Name of Health Plan Administrator (HPA)
-
-
Updated Forms 13441-A require a signature in order to be processed. New enrollments and certain updates require the certification checkbox in Part 2 to be checked (see IRM 3.11.29.9.2).
-
If the signature is not present, do not update the database until a response is received. See IRM 3.11.29.9.6.
-
If a remittance is discovered in any HCTC documentation:
If ... Then ... a) Payable to "US Treasury - HCTC" Notify P&A, then send remittance and payment coupon (if available) to:
US Treasury - HCTC
PO Box 970023
St. Louis, MO 63197-0023b) Payable to another entity: Determine the intent of the payment from the documents in the application packet or correspondence. -
If it is determined remittance is for HCTC, see (9) box a (Payable to "US Treasury-HCTC" ).
-
If it is determined remittance is not for the HCTC, see IRM 3.8.46.1 Discovered Remittances.
-
Elevate to P&A if unable to determine type of remittance.
-
-
Before entering Form 13441-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update, into the database, search for an existing application from the participant already in the database.
-
If the applicant is already in the database:
And... Then... 1) The documents are a response to correspondence and the status of the applications is "Waiting for supporting documentation" -
Enter the requested items into the database
-
Change any information in the database the applicant changed in the response
2) The documents are a response to correspondence and the status of the application is "Cancelled-Ineligible" Refer to HCTC Coordinator 3) The document is not a response to correspondence and doesn’t change the information in the database Consider the Form 13441-A a duplicate and associate it with the original Form 13441-A. See IRM 3.11.29.13, Correspondence. 4) The document is not a response to correspondence; however, it changes information in the database and the status of the application isn’t "Declined," "Cancelled-Ineligible," or "Enrolled" -
Revise the affected information in the database and modify the applicant’s status, if needed
-
Associate the response with the original application
-
Consider the submission a superseding or supplementary Form 13441-A
-
-
If the applicant is not yet in the database, determine which name should be listed as the applicant in the database:
If And Then The eligible recipient is the policy holder Enter the record under the eligible recipient The eligible recipient is not the policy holder The eligible recipient is covered on the policy Enter the record under the policy holder’s name from Part 4 and enter the eligible recipient as a family member in part 3. The eligible recipient is not the policy holder The eligible recipient: -
Is not covered on the policy
-
Is currently eligible for HCTC. See IRM 3.11.29.9.1.1, Determining Eligibility.
Enter the record under the policy holder’s name indicated in Part 4 and see information on separate coverage below. The eligible recipient is not the policy holder The eligible recipient: -
Is not covered on the policy
-
Is divorced from the applicant or is not currently eligible for HCTC. See IRM 3.11.29.9.1.1, Determining Eligibility.
See IRM 3.11.29.15, Qualifying Family Member Participant, for information on determining QFMP eligibility and database entry. -
-
If the eligible recipient and the QFM(s) have separate coverage and Participant Identification Numbers are not already established for each:
If ... Then ... A separate Part 4 is provided for each individual with separate coverage -
Detach family member’s Page 3 (Part 4) from the original application. The family member needs to submit a separate Part 4 only. They do not need to submit a separate Form 13441-A.
-
Enter information as a separate record to establish a new PIN for the family member who has a separate health plan.
-
Edit new family member’s PIN, above Part 4: Health Plan Information, in right corner and process the application.
-
Edit action trail per IRM 3.11.29.4, HCTC Program General Information.
A separate Part 4 is not provided -
Enroll any participant with complete information provided.
-
Correspond for missing Part 4 with Letter 4540, paragraph 13, with the following fill-in: You indicated that you have a separate qualified plan. Please provide a copy of page 4, Form 13441-A, and use Part 4 to provide your health insurance information.
-
-
If the record is being established under someone other than the eligible recipient, edit the file as follows:
-
Edit the eligible recipient in Part 1, if not already present.
-
Edit the policy holder in Part 4, if not already present.
-
Include the name entered into the database beside the PIN in the top right corner of Form 13441-A.
-
Part 3 will be completed normally if there is more than one person on the policy.
-
-
Enter the received date and participant provided information from Part 1: Your General Information of Form 13441-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update, into the relevant fields of the database.
-
The fields for the HCTC Database, Part 1, General Information, are as follows; see (3) below for exceptions and requirements:
Field Items Format Length Required IRS Received Date Stamp Numeric 8 Yes First Name Alphanumeric 25 Yes Middle Name Alpha 25 No Last Name Alphanumeric 35 Yes Suffix Alphanumeric 10 No Social Security Number Numeric 9 Yes Date of Birth Numeric 8 Yes Primary Phone Number Numeric 10 No Alternative Phone Number Numeric 10 No Mailing Address Line 1 Alphanumeric 55 Yes Mailing Address Line 2 Alphanumeric 55 No City Alpha 30 Yes State Alpha 2 Yes Zip Code Numeric 15 Yes -
Certain fields have additional requirements and/or restrictions:
-
Received Date (New enrollments only): If the received date is missing, invalid, or illegible, see IRM 3.11.29.4. Do not change this field if updates are received.
-
First Name/Middle Name/Last Name: Do not abbreviate. Type as written until you reach the end of the field.
-
Social Security Number (SSN): If the SSN on Form 13441-A is invalid and cannot be located, research CC INOLES. If still unable to confirm, then elevate to HCTC Coordinator. Do not enter the record into the database until a valid SSN has been identified.
-
Mailing Address Line 1 / Mailing Address Line 2:
- If mailing address is missing/incomplete, perfect Form 13441-A from the database. For a new enrollment, or if no current address appears in the database, see IRM 3.11.29.13, Correspondence.
- If mailing address is invalid or illegible, perfect the defective elements (house number, street name, apartment number, etc.) using the envelope or attachments. If the address on the envelope or attachments does not appear to be the same address as Form 13441-A, do not perfect based on this information.
- If both a PO Box and a street address are present, enter the street address in the Mailing Address Line 1 field, and the PO Box in the Mailing Address Line 2 field. -
Zip Code: Do not correspond for a missing zip code, but review the attached documents, envelopes, and/or https://www.usps.com/ to determine the correct zip code.
-
-
Except as specified by (3) above, if any required information is missing, invalid, or illegible, perfect it with information from the file. Circle out any incorrect information, edit the perfected information onto Form 13441-A, and enter into the database. Correspond per IRM 3.11.29.13, Correspondence if information cannot be perfected.
-
If any non-required information is missing, invalid, or illegible, it is not required to perfect. Invalid or illegible information must be circled out. Do not correspond for non-required information.
-
When processing new enrollments, an eligibility indicator appears after the SSN is entered. See IRM 3.11.29.9.1.1, Determining Eligibility.
-
After the SSN has been entered, the database will use the TIN-V process to validate and auto-fill the date of birth and address information into the database.
-
If the SSN fails TIN-V, the status will change to either" Ineligible:Could Not Validate TIN at This Time" or "Cancelled - Ineligible: TIN Validation Failure," and the application must be elevated to P&A. When elevating to P&A, include the complete file and an IDRS screen shot of the CC INOLES screen.
-
Eligibility for the HCTC is restricted to two groups of individuals.
-
Individuals who are eligible for benefits under the program Trade Adjustment Assistance (TAA) because of a qualifying job loss and receive benefits through the Trade Readjustment Allowance (TRA), Reemployment Trade Adjustment Assistance (RTAA), or Alternative Trade Adjustment Assistance (ATAA).
- TRA is a weekly cash payment for workers no longer eligible for unemployment benefits
- RTAA is a wage supplement for workers who are 50 or older and certified eligible under the terms of the TAA and find employment at a lower wage
- ATAA is a wage insurance like RTAA -
Individuals who are between 55 and 64 years old, whose defined benefit pension plans were taken over by the Pension Benefit Guaranty Corporation (PBGC) and are not enrolled in Medicare.
-
-
An individual is eligible for the HCTC on the first day of a month if the individual received a TAA benefit for any day in that month or the month before.
-
Only individuals who receive cash benefits through the TRA, RTAA, or ATAA may be certified eligible for the HCTC. Individuals who receive non-cash benefits, such as assistance with looking for a job, aren’t eligible for the HCTC.
-
To determine the applicant’s eligibility for the HCTC, the database checks the record created from Form 13441-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update, against information from the Department of Labor (DoL) and PBGC. The Enrollment Team receives eligibility files from the DoL daily and the PBGC monthly.
-
Enter the applicant’s SSN into the database. If the eligibility indicator "Individual is Eligible (Code 00)" appears, proceed with creating the record.
-
If after entering the applicant’s SSN into the database, the eligibility indicator does not appear:
-
Verify the SSN with CC INOLES in IDRS.
- If the SSN on Form 13441-A doesn’t belong to the applicant, search IDRS for the valid SSN with CC NAMES or within the supporting documentation.
- If the applicant entered the wrong SSN on Form 13441-A, replace the incorrect SSN in the database with the valid SSN retrieved from CC NAMES or from the supporting documents. Write the correct SSN in the margin to the left of the box for the SSN.
- Proceed with creating the record in the database. -
Verify a letter of eligibility from the DoL, PBGC, or relevant Form 1099-R, Distributions from Pensions, Annuities, Retirement or Profit-Sharing Plans, IRAs, Insurance Contracts, etc., is present.
- If present, consider the applicant eligible and proceed with processing Form 13441-A. Perfect the eligibility type (TAA/PBGC) in Part 2 of Form 13441-A to match the supporting documentation provided.
- If not present, see IRM 3.11.29.13, Correspondence.
-
-
An applicant with an IRSN or ITIN is ineligible for the HCTC. If the applicant’s TIN is an ITIN or IRSN:
-
Do not enter the Form 13441-A into the database.
-
Send correspondence Letter 4540 to the participant. See IRM 3.11.29.13.4, Correspondence, Letter 4540.
-
Choose Paragraph 13 with the following fill-in: IRSN or ITIN is ineligible for the HCTC.
-
Return Form 13441-A and all supporting documentation to the applicant.
-
-
An applicant is not eligible after becoming eligible for Medicare at age 65. Correspond using letter 4540 and include the following open paragraph: "You or a family member is eligible to enroll in Medicare." See IRM 3.11.29.13.4, Correspondence, Letter 4540.
-
Enter the information from Part 2: Confirm Your Eligibility of Form 13441-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update, into the relevant fields of the database and update the QFMP information, if applicable.
-
There are three steps to confirm participant eligibility:
-
Confirming the participant is eligible through either PBGC or TAA
-
Confirming the participant meets general requirements
-
Confirming if the participant is a Qualifying Family Member Participant. See IRM 3.11.29.15, Qualifying Family Member Participant (QFMP).
-
-
For statement one, "Check the box that applies to you to certify that the statement is true" , if neither or both boxes are checked:
And Then 1. Either are present: -
An official letter from the Pension Benefit Guaranty Corporation (PBGC) stating that the applicant received a benefit
-
Form 1099-R showing a benefit paid by the PBGC
Select the PBGC button on the screen 2. Either are present: -
An official letter from the Department of Labor (DoL) states that the applicant is eligible for the trade adjustment benefits
-
A letter from a state workforce agency (SWA) or employment office states that the applicant is eligible for trade adjustments benefit
Select the TAA, ATAA, or RTAA button on the screen 3. Neither box 1 nor box 2 above applies. See IRM 3.11.29.13, Correspondence 4. Both box 1 and box 2 above applies. Select the PBGC button on the screen -
-
If the certification checkbox "I certify that all of the following statements are true for me and my qualified family member" is not checked:
-
On a new enrollment, see IRM 3.11.29.13, Correspondence.
-
On an updated Form 13441-A, review the nature of the changes requested. The certification checkbox must be marked if either are true:
- Changes to the covered individuals on the policy (adds, subtracts, or replaces). See IRM 3.11.29.9.3, Inputting Form 13441-A, Part 3: Family Member Information.
- Changes to the health plan vendor in Part 4. See IRM 3.11.29.9.4, Inputting Form 13441-A, Part 4: Health Plan Information.
-
-
Select the third box and edit QFMP dates based on Medicare eligibility when the participant is enrolling as a QFMP. See IRM 3.11.29.15, Qualifying Family Member Participant (QFMP).
-
The database was updated on October 16, 2018, to include the QFMP fields. When updating records entered in the database prior to the update, the QFMP fields can be perfected, but it is not required. Correspondence should not be issued to perfect these fields.
-
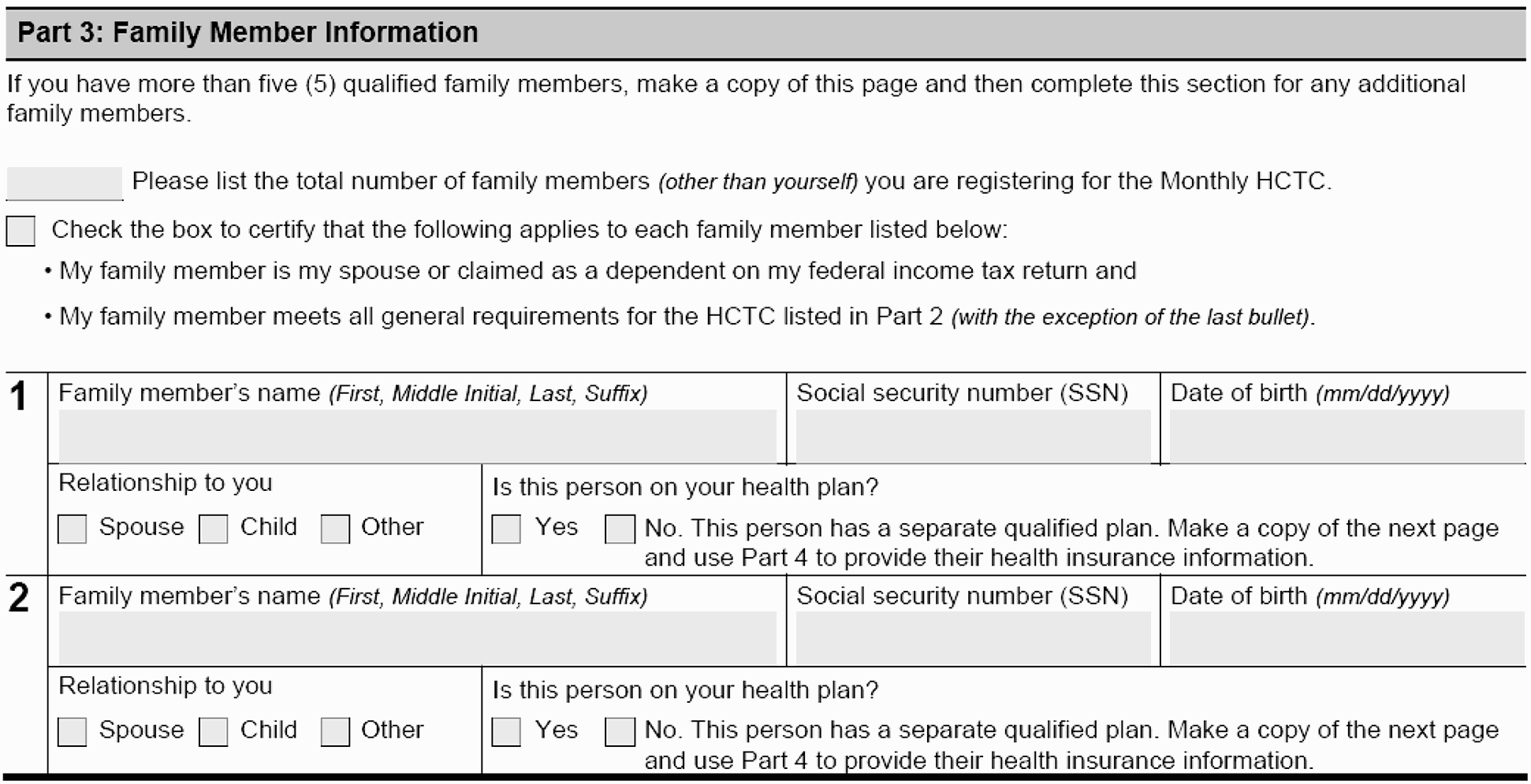
In Part 3: Family Member Information of Form 13441-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update, the applicant reports family members (other than themselves) registering for the HCTC.
-
For special circumstances regarding family members:
-
If the applicant is requesting enrollment as a Qualifying Family Member Participant (QFMP) who is eligible due to the Medicare enrollment, death, or divorce of the eligible recipient, see IRM 3.11.29.15, Qualifying Family Member Participants.
-
If the applicant is requesting enrollment as a Qualifying Family Member (QFM) of the eligible recipient, but the eligible recipient is not the policy holder or has a separate policy, see IRM 3.11.29.9 to determine which individual the record should be created under.
-
-
If there is no family member information in Part 3, select "No" on the Family Member Information screen of the database for "Does the applicant have qualified dependents?"
-
If family member’s information appears in Part 3, select "Yes" on the Family Member Information screen of the database for "Does the applicant have qualified dependents?"
-
Enter available information from Part 3: Family Member Information of Form 13441-A, into the relevant fields of the HCTC database. The database prompts are as follows:
Family Member Item Required a. First Name Yes b. Middle Initial No c. Last Name Yes d. Suffix No e. Family member’s relationship to applicant No f. Social Security Number Yes g. Date of Birth No h. Is this person on the applicant’s health plan? Yes -
The HCTC Database does not currently accept ATINs/ITINs for family members. If the TIN can be verified with IDRS, leave the Social Security Number field of the database blank but enter all other information.
-
If any required information is missing, invalid, or illegible, correct with relevant information found in the supporting documentation. Circle out any incorrect information, edit the perfected information onto Form 13441-A, and enter into the database. If the required information can’t be perfected, see IRM 3.11.29.13, Correspondence.
-
If any non-required information is missing, invalid, or illegible, it is not required to perfect. Invalid or illegible information must be circled out. Do not correspond for non-required information.
-
If the applicant responds "No" to "Is this person on the applicant’s health plan?" a separate Part 4 with family member’s Health Plan Information must be provided. See IRM 3.11.29.9.
-
If the applicant indicates more than five family members, an additional copy of Form 13441-A, Part 3 must be attached. If not attached, see IRM 3.11.29.13, Correspondence.
-
In Part 4: Health Plan Information, the applicant reports information about the health plan provider and information which affects their monthly payment. Enter provided information from Part 4 of Form 13441-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update, into the relevant fields of the HCTC database.
-
Each policy holder for each Part 4 must have their own record. If Form 13441-A indicates that family members have separate coverage, see IRM 3.11.29.9 for details.
-
The HCTC Coordinator will review the HPA Vendor Number, Member ID, Group ID, and Policy or Plan ID on all new enrollments and re-enrollments or if the participant indicates a change to their vendor information.
-
The HCTC Coordinator will attach a Vendor Verification Form to the bottom right of Part 4 if providing missing/corrected information.
-
If the HCTC Coordinator is unable to determine the vendor number and at least one of the other fields, elevate to HQ
-
-
Where present, the entries on the Vendor Verification Form will take precedence over the entries on Form 13441-A.
-
If the participant submits an update to change the Vendor, Member ID, Group ID, and/or Policy or Plan ID and no updated Vendor Verification is present, refer to the HCTC Coordinator for determination. If the HCTC Coordinator determines the vendor is not enrolled, correspond per IRM 3.11.29.13.4, using paragraph 12.
-
The fields for the HCTC Database, Part 4, Health Plan Information, are as follows; see (7) below for exceptions and requirements:
Health Plan Item Required a. Vendor Name Yes b. Vendor Number Auto populated c. Effective Date of Coverage (MMDDYYYY) Yes d. Health Plan ID Number No e. Member ID* See Note f. Group ID* See Note g. Policy or Plan ID* See Note h. Policy Holder’s First Name Yes i. Policy Holder’s Middle Initial No j. Policy Holder’s Last Name Yes k. Policy Holder’s Suffix No l. Social Security Number Yes m. Total Monthly Premium (line 1) Yes n. Total number of people on policy (line 2) No o. Number of family members on policy who are not qualified for the HCTC (line 3) No p. Monthly premium amount for family members not qualified for the HCTC (line 4) No q. Other Health Benefits Amount (line 6) No r. Total HCTC (line 5) Auto populated s. Monthly HCTC Payment (line 7) Auto populated t. Total Government Payment Auto populated -
Certain fields have additional requirements and/or restrictions:
-
If the effective date is blank, research the packet for an indication of when HCTC Eligibility begins. If none is found enter the current date.
-
At least one of the following is required: Member ID, Group ID, or Policy ID. Elevate to the HCTC Coordinator if none are present. If any of these fields exceed the field length, refer to HCTC Coordinator for determination. Coordinator will reorder entries between these fields if possible; otherwise, TE will be instructed to enter as much of the entry as possible in each field.
-
-
Use the table below to correct common participant errors:
On Form 13441-A, if... And... Then... a. The vendor is changing There is an End Date for COBRA coverage in the database which is not being updated Refer to the HCTC Coordinator for determination. b. The policy holder is the applicant The policy holder’s SSN in Part 4 differs from the SSN in Part 1 Replace the SSN in Part 4 with the valid SSN from Part 1 of Form 13441-A c. Line 2, "Total number of people on this policy" is blank No family members appear in Part 3 Enter "1" onto line 2, "Total number of people on policy" d. Line 2, "Total number of people on this policy" is greater than "1" No family members appear in Part 3 See IRM 3.11.29.13, Correspondence e. Line 2, "Total number of people on this policy" is blank Family members appear in Part 3 Enter the sum of the applicant plus the family members from Form 13441-A, Part 3 onto line 2, "Total number of people on this policy" f. Line 3, "Number of family members on this policy who are not qualified for HCTC" is greater than zero Line 4 "Monthly premium amount for family members who are not qualified for HCTC" is blank No correction is required. Enter lines 3 and 4 into the database as given. g. Line 4 "Monthly premium amount for family members not qualified for the HCTC" is greater than zero Line 3 "Number of family members who are not qualified for the HCTC" is blank or zero Add the amount on line 4 to any existing amount on Line 6, "Other health benefits amount" . -
Other Benefits (or Other health benefits) refer to premiums for insurance which is not eligible for the HCTC (dental, vision, etc.). This amount will be automatically added to the participant’s Total HCTC (27.5% medical premium payment) to determine the participant’s monthly payment amount.
-
Do not enter Consolidated Omnibus Budget Reconciliation Act (COBRA) fields into the HCTC database if the participant is PBGC eligible.
Note:
This includes cases when the participant indicated that they were eligible as both TAA and PBGC recipients.
The database prompts are as follows:COBRA Information Required a. Former Employer No b. Former Employer’s HR Phone Number No c. Start Date for COBRA Coverage (mm/dd/yyyy) No d. End Date for COBRA Coverage (mm/dd/yyyy) No e. Lifetime Benefit checkbox No -
If the "Check here if you are changing from a COBRA Health Plan to a non-COBRA health plan" box is checked, delete previously entered COBRA dates in the database.
-
If the Lifetime Benefit checkbox is selected:
-
If the TAA box in Part 2: Confirm Your Eligibility of Form 13441-A is not checked, refer to the HCTC Coordinator.
-
Circle out any End Date for COBRA Coverage. Delete the COBRA End Date from the database, if present.
-
Change the participant’s birth year to 2000 in the database. Add the actual birth year in a comment stating "Lifetime Benefits: Actual birth year 19xx"
-
-
If any required information is missing, invalid, or illegible, correct with relevant information found in the supporting documentation. Circle out any incorrect information, edit the perfected information onto Form 13441-A, and enter into the database. If the required information can’t be perfected, see IRM 3.11.29.13, Correspondence.
-
If any non-required information is missing, invalid, or illegible, it is not required to perfect. Invalid or illegible information must be circled out. Do not correspond for non-required information.
-
In Part 5: Account Accessibility of Form 13441-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update, the applicant can designate a Third-Party to have access to their account information.
-
Enter information from Part 5: Account Accessibility of Form 13441-A, if a five-digit numerical Personal Identification Number (PIN) is provided.
-
No correspondence is necessary if any of the information is missing or incomplete.
-
In Part 6 of Form 13441-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update, the applicant signs the form. Do not process changes to Form 13441-A without a signature.
-
If Form 13441-A is unsigned and changes are requested:
-
Do not update the database.
-
Correspond with Letter 4540, paragraph 5 and 5e.
-
Return the unsigned Form 13441-A and all related documents to the applicant.
-
Include a blank Form 13441-A signature page with the correspondence if Part 6 is missing from the application, if the signature is "X’d," or if the signature is lined through.
-
-
If the signature is missing and there are no requested changes, comment the file and do not correspond for missing signature. See IRM 3.11.29.13 ,Correspondence, if the account is currently in a non-enrolled status due to missing information.
-
The signature must appear under the jurat — "Under penalty of perjury…" —and above the phrase "Privacy Act and Paperwork Reduction Act Notice." If Form 13441-A is signed outside this area, treat as unsigned.
-
Faxed, digital, or photocopied signatures are acceptable.
-
Accept a signature by a third party only with a power of attorney (POA):
-
Form 2848 , Power of Attorney and Declaration of Representative, names the third party and may be present in the packet.
-
If Form 2848 is not part of the packet, look for the POA with CC CFINK.
-
If the applicant hasn’t granted power of attorney to the person who signed the Form 13441-A, treat as unsigned.
-
-
If the signature section is "X’d" or lined through, either pre-printed or manually, treat as unsigned.
-
If you enter Form 13441-A with a missing signature in error into the database:
-
Set the eligibility status to "Processing— Waiting for Supporting Docs."
-
Add a comment into the database stating the application was entered in error without a signature.
-
-
There are several statuses available in the HCTC database for participants depending upon their application. If you are unable to change a status on an application, then refer to HCTC Coordinator for elevation to P&A.
-
Anytime a record is updated, use the following chart to determine the status for the application.
Note:
Any status change which moves a participant out of "Enrolled" status should be elevated to P&A.
If ... Then ... Applicable Letter The application packet is complete and acceptable and the applicant is eligible Move to Complete IRM 3.11.29.13.5, Letter 4545, HCTC Enrollment Letter You are reviewing an application Move to Quality Review Quality Review has been performed and the participant is able to be enrolled Move to Enrolled Participant’s health plan is not enrolled in the HCTC AMPThis status will always take priority if we are corresponding for a HPA Vendor in addition to anything else. Processing—HPA Vendor Num Not Avail IRM 3.11.29.13.4, Letter 4540, HCTC Candidate Eligibility Denial Participant’s health plan is not qualified for the HCTC. Cancelled-Ineligible IRM 3.11.29.13.4, Letter 4540, HCTC Candidate Eligibility Denial Information on Form 13441-A or supporting documentation is defective, missing, incomplete, invalid, or illegible and the applicant is eligible. Processing—Waiting for Supporting Docs. IRM 3.11.29.13.4, Letter 4540, HCTC Candidate Eligibility Denial The application packet is incomplete or unacceptable, and the applicant is eligible but didn’t reply or inadequately replied to correspondence send Letter 4540 with the relevant correspondence paragraphs.See IRM 3.11.29.13.4, Letter 4540, HCTC Candidate Eligibility Denial. Cancelled -Ineligible IRM 3.11.29.13.4, Letter 4540, HCTC Candidate Eligibility Denial The participant has been enrolled and is now requesting removal from the program Cancelled—Ineligible IRM 3.11.29.13.1, Letter 3772, End of Program Letter COBRA insurance has expired Cancelled—Ineligible IRM 3.11.29.13.4, Letter 4540, HCTC Candidate Eligibility Denial The participant had been enrolled and is no longer eligible Cancelled—Ineligible IRM 3.11.29.13.1, Letter 3772, End of Program Letter None of the above scenarios are applicable Refer to the HCTC coordinator -
When removing an applicant from an enrolled status, do not delete existing information from the database unless specifically instructed. The most recent information is retained.
-
The following statuses are no longer in use:
-
Processing-HPA Vendor Num Avail: Should not appear in database.
-
Ineligible: May appear in database, replace with Cancelled-Ineligible if updating the record.
-
Cancelled-Permanent Ineligibility: May appear in database, replace with Cancelled-Ineligible if updating the record.
-
-
Following are several statuses that are systemically generated by the HCTC database. If you believe a systemically generated status is incorrect, elevate to P&A.
-
Form received
-
Inactive
-
Cancelled: Permanent Ineligibility - Over 65
-
Ineligible - Over 65
-
Cancelled: Ineligible - COBRA End Date Expired
-
Ineligible - COBRA End Date Expired
-
Cancelled: Ineligible - Prison File Match
-
Ineligible: Could Not Validate TIN at This Time
-
Cancelled - Ineligible: TIN Validation Failure
-
Ineligible - QFM End Date Expired
-
Cancelled: Ineligible QFM End Date Expired
-
-
For the statuses in the table below, the database will automatically unenroll the participant. The participant must be notified 45 days prior to the loss of eligibility based on date entries in the fields listed in the table. See IRM 3.11.29.13.1, Letter 3772, End of Program Letter.
Status Expiration Determined By Cancelled: Permanent Ineligibility - Over 65 Date of Birth Ineligibility - Over 65 Date of Birth Cancelled: Ineligible - COBRA End Date Expired End Date for COBRA coverage Ineligible - COBRA End Date Expired End Date for COBRA coverage Cancelled: Ineligible - QFM End Date Expired End Date for QFM Ineligible - QFM End Date Expired End Date for QFM -
When the database moves a previously enrolled participant into the status "Cancelled: Ineligible - Prison File Match" , elevate to P&A for review.
-
Clerks review each Form 13441-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update, before releasing to Files and/or the storage area. They verify that all pages of Form 13441-A are present and supporting documents are attached.
-
Each packet with Form 13441-A may contain one or more of the following:
-
The original Form 13441-A
-
An updated Form 13441-A
-
Required supporting documentation: a copy of the participant’s health insurance bill dated within the last 60 days
-
A copy of any correspondence sent to the applicant
-
Any correspondence sent by or on behalf of the applicant
-
-
Clerks verify that the PIN (Participant Identification Number) on the Enrollment letter matches the PIN on the first page of Form 13441-A.
-
In the Batch Block Tracking System (BBTS), Clerks release Forms 13441-A and associated documents to Files and/or the storage area.
-
Place each batch of Forms 13441-A, along with the Form 9856, Attachment Alert, and two copies of Form3210, Document Transmittal, for the batch, into a gusset folder. On the tab of the gusset folder, write the range of PINs, the program name "HCTC," and the tax year of the applications.
-
Route Forms 13441-A numbered with a PIN to Files or a designated storage area at the Austin Submission Processing campus to be held until retirement.
-
Retain Forms 13441-A at the Austin processing center for six (6) years, beginning in 2016. After the end of the sixth year, retire Form 13441-A to the Federal Record Center (FRC) for an indefinite period. See IRM 3.11.29.25, Record Retention Requirements.
-
Include an Application Identification Sheet (AIS) and highlight the correct PIN. The AIS is used to attach documents to the applicant’s packet.
-
The Enrollment Team is responsible for sending the following letters.
Letter Title Purpose 3772 End of Program Letter To cancel participant’s HCTC registration or notify the participant of upcoming systemic unenrollment. 4510 HCTC Reimbursement Request – Denial To deny request for reimbursement (Form 14095) 4511 HCTC Reimbursement Request - Insufficient Documentation Participant provided insufficient documentation (Form 14095) 4540 HCTC Candidate Eligibility Denial To notify participant of ineligibility and/or missing documentation. 4545 HCTC Enrollment Letter To notify participant of confirmed enrollment 5758 Health Coverage Tax Credit Enrollment in Process To acknowledge receipt of application. For use only with explicit management approval. 5945 HCTC Reimbursement Approval Notifies participant request was approved (Form 14095) 5974 Annual HCTC Vendor Renewal Notification To remind HPA/TPA to annually certify to receive ACH payments 6009 Refund of HCTC Payments To notify participant of refund of HCTC payments 6011 Return of HCTC Funds To request funds from a participant (HQ Only) -
Do not save any correspondence containing participant’s Personal Identifiable Information (PII) to your desktop or personal storage drive.
-
Remove all editing marks prior to returning any document to an applicant.
-
When it is necessary to correspond with taxpayers, correspondence should be professional (i.e., correct spelling, punctuation, and grammar).
-
Correspondence letters are available through the HCTC SharePoint.
-
Correspond only after you have entered the entire Form 13441-A into the HCTC database.
-
Enter comments into the HCTC database, including what letter was sent and why the letter was sent (correspondence conditions).
-
All correspondence must include the participant’s Participant Identification Number.
-
Address all decedent correspondence to "Estate of" and the decedent’s name. (e.g., Estate of John Smith)
-
One copy of all correspondence is attached to the applicable applicant package in Received Date order with the oldest stapled to the top. See IRM 3.11.29.4, HCTC Program General Information.
-
All letters are subject to review by the Improvement Team.
-
Retrieve E-faxes daily. Check the E-fax folder daily for replies/missing information. Print the reply and associate it with the original submission on the suspense wall.
-
Each correspondence letter may trigger a change in the status of the application. See IRM 3.11.29.10, Setting the Status of the Application.
-
Allow applicant 45 days for responding to correspondence. A reply is late on the 46th day after correspondence.
-
Duplicate Form 13441-A: If a Form 13441-A is received which appears to be a duplicate of the current 13441-A:
-
Review the Form 13441-A thoroughly for any changes.
-
Review any supporting documentation or correspondence for indications that a change was intended or that this is a reply to prior correspondence.
-
Verify that the signature date, if any, is the same.
-
-
If, after review, the Form 13441-A still appears to be a duplicate, process the Form 13441-A normally, but do not re-issue any correspondence. Comment the database to indicate that a duplicate 13441-A was received, and no correspondence was issued.
Exception:
If the received date of the duplicate is greater than 30 days from the received date of the current form and the account is in a non-enrolled status due to missing information, process and correspond as normal to ensure the participant is aware of any unresolved issues related to their account.
-
Undeliverable Correspondence: When undeliverable correspondence is received, research the database, the file, and/or IDRS for an alternative address.
-
If an alternative address is found, reissue the correspondence. Comment the database with the address used and date resent. Do not change the address in the database without Form 13441-A or a 4442 instruction (see IRM 3.11.29.14).
Note:
https://www.usps.com should be used to perfect missing/invalid elements of the address, if applicable.
-
If a better address is not found, comment the database to indicate which letter was returned undeliverable and that no alternative address was found. Do not reissue letter.
-
-
Letter 3772, End of Program Letter, informs participants they have been cancelled from the HCTC program, or notifies them that they will be systemically unenrolled at a future date. See Exhibit 3.11.29-1. See also IRM 3.11.29.10, Setting the Status of the Application.
-
Monthly, the HCTC Coordinator will create a list of applicants who will be systemically unenrolled within the next 60 days due to Medicare eligibility, COBRA expiration, or QFMP end date. Issue Letter 3772 to notify identified participants that they will be unenrolled/ineligible.
-
If the change is effective immediately, change the status of the application to "Cancelled-Ineligible." . Do not change the status if participant will be unenrolled systemically at a future date.
-
Along with the standard address, date, and last four digits of the participant’s SSN, enter the following:
-
Participant Identification Number (PIN) beside Dear HCTC Program participant
-
Open paragraph with HQ pre-approved text, if provided.
-
-
Letter 4510, HCTC Reimbursement Request – Denial, is a denial letter for the reimbursement request for the HCTC Advance Monthly Program. See Exhibit 3.11.29-2. Letter 4510 will be sent only when instructions are received from P&A.
-
There will be no status change when sending Letter 4510.
-
Along with the standard address, date, and last four digits of the participant’s SSN, enter the following (provided by P&A):
-
Participant Identification Number (PIN) beside "Dear HCTC Program participant"
-
Month(s) the reimbursement is requested in the first paragraph
-
Amount of the reimbursement request in the first paragraph
-
Reason for denial (check box entry)
-
Open paragraph with HQ pre-approved text, if needed
-
-
Letter 4511, HCTC Reimbursement Request - Insufficient Documentation, is sent to request documentation for the reimbursement request Form 14095, The Health Coverage Tax Credit (HCTC) Reimbursement Request Form. See Exhibit 3.11.29-3. Letter 4511 will be sent only when instructions are received from P&A.
-
There will be no status change when sending Letter 4511.
-
Along with the standard address, date, and last four digits of the participant’s SSN, enter the following (provided by P&A):
-
Participant Identification Number (PIN) beside "Dear HCTC Program Participant"
-
Open paragraph with HQ pre-approved text, if needed
-
-
Letter 4540, HCTC Candidate Eligibility Denial, notifies participants their HCTC eligibility has not been processed or they are missing or have incomplete documentation. See Exhibit 3.11.29-4. See IRM 3.11.29.10, Setting the Status of the Application.
-
If the participant is currently enrolled, refer to HCTC Coordinator prior to corresponding for missing information as some information can be obtained through vendor outreach.
-
Change the status in the database to one of the following, depending on the circumstances.
-
Processing—Waiting for Supporting Documentation
-
Processing—HPA Vendor Not Avail
-
Cancelled-Ineligible
-
-
Letter 4540 is customizable with 13 selectable paragraphs on the following topics. Multiple paragraphs may be selected to appear in the same letter.
-
Paragraph 1 - Dependent status
-
Paragraph 2 – Disqualifying health insurance coverage
-
Paragraph 3 – Age requirement (PBGC only)
-
Paragraph 4 – Imprisonment
-
Paragraphs 5a-5e – Incomplete registration form
-
Paragraph 6 – Missing supporting documents
-
Paragraph 7 – Spousal coverage
-
Paragraph 8 – Participant eligibility
-
Paragraph 9 – Family member eligibility – Insufficient documentation
-
Paragraph 10 – Family member eligibility – Unable to confirm eligibility
-
Paragraph 11 – Family member eligibility – You are not eligible
-
Paragraph 12 – Unable to verify Health Plan Administrator (HPA) set up
-
Paragraph 13 – Miscellaneous missing information
-
-
If signature is missing, return the unsigned Form 13441-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update, and all related documents to the applicant. See IRM 3.11.29.9.6, Inputting Form 13441-A, Part 6: Form Completion.
-
If the signature is" X’d," crossed out, or lined through, either pre-printed or manually, return the original Form 13441-A and all related documents to the applicant with a blank Form 13441-A signature page.
-
If you are not returning Form 13441-A to the applicant, remove the words "Enclosures: Your Form 13441-A" from page 2 of Letter 4540 prior to printing.
-
When an adequate response is received, or if the 45-day suspense period passes with no response, an inadequate response or an incomplete response:
-
For an adequate response in which all required information is present and acceptable, update the information in the database to reflect the applicant’s response. See IRM 3.11.29.10, Setting the Status of the Application.
-
For no response, inadequate response or an incomplete response in which required information is missing or unacceptable:
-
Send Letter 4540 with the relevant correspondence paragraphs.
-
Utilize the open paragraph with HQ pre-approved text.
-
Set the status of the application to Cancelled-Ineligible.
-
-
Letter 4545, HCTC Enrollment Letter, notifies participants that their HCTC eligibility has been successfully processed. See Exhibit 3.11.29-5. Along with the standard address, date, and last four digits of the participant’s SSN:
-
Enter the Participant ID number
-
Enter the Monthly HCTC Payment in the field "Amount due" in the second paragraph
-
-
If the participant is not currently enrolled, change the status in the database to "Complete" .
-
Letter 5758, Health Coverage Tax Credit Enrollment in Process, is used to acknowledge receipt of Form 13441-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update and supporting documents. See Exhibit 3.11.29-6.
-
Do not send this letter without explicit instructions from management.
-
Letter 5945, HCTC Reimbursement Approval, notifies participants that their request for reimbursement on Form 14095, The Health Coverage Tax Credit (HCTC) Reimbursement Request Form, has been approved and they should expect a payment within three weeks. Letter 5945 will be sent only when instructions are received from P&A. See Exhibit 3.11.29-7.
-
Along with the standard address, date, and last four digits of the participant’s SSN, enter the following (provided by P&A):
-
Enter the Participant ID number
-
Enter the reimbursement payment amount in the "$0.00" field in the second paragraph
-
-
Letter 5974, Annual HCTC Vendor Renewal Notification, notifies Health Plan Administrator (HPA) or the Third-Party Administrator (TPA) that they must annually complete a Form 3881-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update, to continue to receive Automatic Clearing House (ACH) payments from the HCTC program. See Exhibit 3.11.29-8. Along with the standard address, date, and last four digits of the vendor’s EIN (in the Taxpayer ID Number box) enter the following:
-
Enter the HPA/TPA name
-
Enter a due date in the "[insert date]" prompt in the third paragraph
-
-
Letter 6009, Refund of HCTC Payments, notifies participants that they will be receiving a refund of payments for applicable months. Letter 6009 will be sent only when instructions are received from P&A. See Exhibit 3.11.29-9.
-
Along with the standard address, date, and last four digits of the participant’s SSN, enter the following (provided by P&A):
-
Enter the Participant Identification number (PIN).
-
Enter the HCTC Program participant name following "Dear HCTC Program participant:"
-
Use the drop-down box to make the appropriate selection of "month" or "months."
-
Enter the name of the appropriate month(s) in the "[enter months]" prompt. Enter exactly as it will appear in the body of the letter.
-
Enter the amount of payment being returned to the participant in the "[123,456.00]" prompt. Include comma separators for thousands (if needed) and cents. Enter exactly as it will appear in the body of the letter.
-
If needed, utilize the open paragraph with HQ pre-approved text.
-
-
Letter 6011, Return of HCTC Funds, is sent by HQ analysts to a participant to request the return of HCTC monies for any of the following reasons:
-
Administrative Error
-
Repayment of Other Benefits
-
Participant Identification Number Mismatch
-
Other
-
-
The HCTC participant is requested to send a check to the HCTC Chief Financial Office (CFO) IRS Beckley Office.
-
Documentation may be sent to the Enrollment Team, by the participant, and should be elevated to P&A.
-
HQ will review the documentation and will send it back to the Enrollment Team to be attached to the participant’s file.
-
Participant correspondence may be received by e-mail, fax, or forwarded from another department for processing. Form 4442 are received from Accounts Management (AM). Participant correspondence and items received from Lockbox (US Bank) should be processed as Forms 4442.
-
When participant correspondence or a Form 4442 is received, review the inquiry.
-
If the request is processable following normal procedures, process and respond as needed. Comment the database, describing any action taken.
-
If a copy of a US Bank rejection letter is received which begins "We have received your HCTC payment; however, we are unable to process your payment for the following reason(s):" , comment the database with the reason for rejection and add to the participant’s file.
-
If the request involves a payment question, Form 1099-H, or is not allowable following normal procedures, elevate to P&A.
-
If a remittance is discovered with participant correspondence, see IRM 3.11.29.8.
-
-
When forwarding Form 4442 to AM, include a copy of any correspondence (member, third party, etc.) to assist customer service representatives (CSRs) when responding back to HCTC participants.
-
Return Form 4442 to the originator if:
-
The person named in Form 4442 isn’t in the database
-
Form 4442 doesn’t provide enough information to determine relevance, intention, or identify the applicant
-
Form 4442 was sent to the Enrollment Team in error
-
-
When P&A issues a substitute Form 4442 with instructions to the Enrollment Team:
-
Process the item(s) as requested.
-
Review the change for any additional actions generated, particularly correspondence criteria. See IRM 3.11.29.13
-
Comment the database with the action(s) taken.
-
Route substitute Form 4442 to QR.
-
-
Due to the potential for specific harm to participants - up to and including lapses of health insurance - it is necessary to expedite some cases through the enrollment/update process. If an expedite request is issued, the document should be hand-walked through the enrollment/QR process before the end of the business day (unless otherwise specified).
-
If correspondence is required on an expedited document, contact P&A and/or HQ to find out if the correspondence issue can be resolved by contacting the participant and/or vendor.
-
If conflicting priorities make expediting the document impossible, P&A and/or HQ must be notified as soon as possible.
-
Most expedite requests will be issued from HQ based on contact from the participant/vendor, but P&A and/or the HCTC Coordinator may make the determination if a potential for specific harm is identified. TEs may refer cases to the HCTC Coordinator for review if they believe it is necessary to expedite.
-
-
Form 4442 must be attached to the back of Form 13441-A. See IRM 3.11.29.4, HCTC Program General Information.
-
A Qualifying Family Member Participant (QFMP) is a family member (spouse or dependent) who may maintain their HCTC enrollment for 24 months after one of the following qualifying events:
-
Eligible recipient is eligible for Medicare.
-
Eligible recipient is deceased.
-
If the QFM is divorced from the eligible recipient.
-
-
A QFMP relies on the eligibility information of the eligible recipient but must meet all other requirements for enrollment.
-
New enrollments should be reviewed for QFMP status. Possible indications that Form 13441-A is related to a QFMP include (but are not limited to):
-
Form 13441-A, General Instructions, box 6 is checked
-
Form 13441-A is filled out for a name other than the eligible recipient
-
Participant correspondence is attached
-
Supporting documentation for QFMP status is present (see below)
-
-
QFMP due to Medicare Eligibility – In most cases, an individual becomes eligible for Medicare the first day of their birth month the year they turn 65. An individual will be treated as HCTC eligible during their entire birth month in which they turn 65 for purposes of computing the HCTC credit for QFMPs during the 24-month QFMP eligibility period.
-
Form 13441-A for enrollment must be completed and signed by either the eligible recipient or the QFMP.
-
One or more of the following must be true:
- Eligible recipient is 65 or older.
- Eligible recipient was previously enrolled and was unenrolled from HCTC AMP due to Medicare eligibility.
- A Medicare enrollment letter, Medicare card, or other documentation of Medicare eligibility is present.
-
-
QFMP due to Divorce – The spouse of the eligible recipient is eligible for enrollment following a divorce. Eligible dependents may be included on either policy.
-
Form 13441-A must be completed and signed by the QFMP.
-
A divorce certificate identifying the eligible recipient (or similar legal documentation) is required and must include the date of divorce
-
-
QFMP due to Death – The spouse and/or dependents of a deceased eligible recipient are eligible for enrollment.
-
Any spouse of the participant (determined at the time of death) is treated as an eligible individual
-
Any individual who was a QFM immediately before such death is treated as an eligible individual
-
The enrollment form must be completed and signed by the QFMP.
-
A death certificate for the eligible recipient, (or similar documentation which includes the date of death) must be present.
-
-
Determine the QFM Start Date field using qualifying event date:
If Then QFMP is eligible due to Medicare In the QFM Start Date field, enter the first day of the following month. QFMP is eligible due to divorce or death and was on eligible recipient’s medical policy on the date of the qualifying event In the QFM Start Date field, enter the first day of the following month. QFMP is eligible due to divorce or death and was on a separate medical policy on the date of the qualifying event In the QFM Start Date field, enter the first day of the qualifying event month. You cannot determine the date of the qualifying event Correspond per IRM 3.11.29.13.4 , Correspondence Letter 4540. The date of the qualifying event does not match the effective date on the form. Refer to the HCTC Coordinator for determination. -
If an individual is identified as a QFMP:
-
Create the database record under the name of the QFMP.
-
Edit the eligible recipient in Part 1, Form 13441-A, if not already present.
-
Edit the policy holder in Part 4, Form 13441-A, if not already present.
-
Include the QFMP name beside the Participant Identification Number in the top right corner of Form 13441-A.
-
If a QFMP was previously enrolled under an eligible recipient, edit an action trail on both forms. Reference the QFMP PIN on the eligible recipient’s form and reference the eligible recipient’s PIN on the new QFMP form in the top left margin.
-
Comment the database with “QFMP of [eligible recipient’s name.]” Include eligible recipient’s PIN, if established. If not established, enter the eligible recipient’s name and birthdate from Form 13441-A, Part 1.
-
Part 3, Family Member Information, will be completed normally if there is more than one person on the policy. Do not include the eligible recipient in Part 3.
-
Complete the QFM information in Part 2: Eligibility in the HCTC database using the information above.
-
The database will calculate an end date of 24 months after the start date.
-
Enter QFMP’s name and PIN to eligible recipient’s record, if present.
-
-
Taxpayers can request 72.5% reimbursement for premiums they paid directly to their administrator while waiting to be accepted into the Advance Monthly Program by using Form14095, The Health Coverage Tax Credit (HCTC) Reimbursement Request Form.
-
General: When a Form 14095 is received in the Enrollment Team:
-
The Enrollment Team will pull the original Form 13441-A and attach to the Form 14095.
-
The HCTC Coordinator will notify P&A as Forms 14095 are received in the unit
-
-
P&A: When a Form 14095 is received, P&A will research eligibility for reimbursement.
-
P&A will identify and elevate to HQ any discrepancies between information recording in the database and information supplied with Form 14095.
-
HQ will determine the cause of the variance. If the cause can be determined, the amount should be corrected to reflect the database amounts when possible.
-
Where HQ cannot determine the cause, the participant is reimbursed based on the attached proof of payment in conjunction with what is on the Form, ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡.
-
If the participant paid less than their total premium amount for any month, the participant is reimbursed the substantiated amount. This includes pro-rated payments and partial payments required due to an unprocessed premium change.
-
If the variance is greater than the tolerance correspondence is needed. See IRM 3.11.29.13, Correspondence.
-
If P&A determines that supporting documentation does support Form 14095, they will submit the claim to HQ for final approval.
-
If P&A determines that supporting documentation does not support Form 14095 claim, they will prepare a Substitute Form 4442, Inquiry Referral, instructing the Enrollment Team to send Letter 4510 or Letter 4511, as appropriate.
-
On the 15th and 30th of each month, after HQ approval, either the P&A Analyst or HQ will forward the spreadsheet to the public mailbox ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ to be processed. If either the 15th or 30th fall on a non-business day, spreadsheet submission takes place on the business day immediately prior.
-
-
Submit the spreadsheet to CFO with the following information:
"The attached spreadsheet represents payment to participants who submitted Forms 14095. The (Month) (15th or 30th), 202X submission to CFO represents a total of $(Amount) for reimbursements of the 72.5% portion of the health insurance."
"Retroactive Refunds, the government portion, Fund R0923HTC"
-
Due to program constraints, Forms 14095 have an annual cutoff of September 30th and will resume after the beginning of the new year. Any reimbursement requests with a Received Date stamp after September 30th will need to be claimed on the participant’s federal tax return using Form 8885, Health Coverage Tax Credit. Forms 14095 with a Received Date stamp after September 30th for the current processing year will be returned to the participant with Letter 4510, using the open paragraph for the September cutoff date. See IRM 3.11.29.13.2, Letter 4510, HCTC Reimbursement Request - Denial.
-
Enrollment Team: After processing is complete, P&A will return forms to the Enrollment Team for batching, correspondence, and comments.
-
The Enrollment Team will prepare the required correspondence indicated by P&A on the substitute Form 4442 and add comments to the HCTC database. P&A will send an email confirmation, to HQonce correspondence is issued. See IRM 3.11.29.13, Correspondence and IRM 3.11.29.4, HCTC Program General Information.
-
Letter 5945, HCTC Reimbursement letter, will be used to approve reimbursed amounts. See IRM 3.11.29.13.7.
-
Letter 4511, HCTC Reimbursement Request - Insufficient Documentation, will be used to request missing information. See IRM 3.11.29.13.3 .
-
Letter 4510, HCTC Reimbursement Request - Denial, will be used to deny ineligible claims. See IRM 3.11.29.13.2
-
-
Attach Forms 14095, supporting documentation, and letters to the back of the participant’s original Form 13441-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update, as instructed in IRM 3.11.29.4, HCTC Program General Information
-
P&A will verify the following from Form 14095, The Health Coverage Tax Credit (HCTC) Reimbursement Request Form, with information in the HCTC database.
-
The participant is eligible for the requested reimbursement month(s) while they were enrolling in the Advance Monthly Program (AMP) or chose not to be in the AMP program. Reimbursement can only be for January through September of the current calendar year.
-
Participant may be eligible for the requested reimbursement month(s) after they were enrolled in the program, in limited circumstances. If participant is requesting reimbursement for month(s) after enrollment in the HCTC AMP, refer to HQ for determination.
-
The requested reimbursement months were for months the participant did not receive monthly program payments through their Health Plan Administrator (HPA) or Third Party Administrator (TPA).
-
-
P&A will verify that a health insurance bill, payment coupon, or similar documentation from the Health Plan Administrator (HPA) or Third Party Administrator (TPA) is present for the months identified in Part 2 of Form 14095, The Health Coverage Tax Credit (HCTC) Reimbursement Request Form. These documents must contain the following information:
-
Name of the participant
-
Social Security Number (SSN) of the policy holder if different from requestor
-
Name of health plan
-
Monthly premium amount
-
Dates of coverage
-
Health plan ID number including one of the following:
- Member ID
- Group ID
- Policy ID
- Plan ID
-
-
Proof of payment must indicate the amount paid and to whom it was paid. Proof of payment includes evidence of full payment of premiums, such as bank statement, copies of checks, credit card statements, or receipts for money orders.
-
If it is unclear the available documentation is sufficient to support the claim, refer the claim to HQ for determination. Include a scan of all supporting documents.
-
Form 14095, The Health Coverage Tax Credit (HCTC) Reimbursement Request Form, must be signed. If form 14095 is not signed:
-
Correspond with Letter 4511, HCTC Reimbursement Request - Insufficient Documentation. See IRM 3.11.29.13.3.
-
Leave comments in the HCTC database specifically stating what is missing.
-
Attach letter to base file.
-
-
Replies to correspondence for Form 14095, The Heath Coverage Tax Credit (HCTC) Reimbursement Request Form, should be elevated to P&A. This includes participants appealing the decision or requesting additional information on the determination.
-
P&A will review replies and return forms to the Enrollment Team for batching and correspondence.
-
Each month the Department of Treasury transmits 100% of the insurance premium payments to the Health Plan Administrator (HPA) or Third-Party Administrator (TPA) through a payment file for all enrolled participants associated with the HPA/TPA’s vendor number. This payment file is used to reconcile payments for each participant.
-
If after reconciliation it is discovered participants had an unapproved vendor, duplicate payments, misapplied payments, were using an incorrect Participant Identification Number (PIN), among other instances, then HPA/TPA/Participants may be refunded their portion of the insurance premium.
-
Payment reconciliation is handled on a case-by-case basis by HQ with two different processes: participants and vendors.
-
For participants, the reimbursement process is completed by HQ on a spreadsheet and is submitted to Chief Financial Office (CFO).
-
When submitting the spreadsheet to CFO, use the following information:
"The 1034 spreadsheet represents HCTC payments to participants based on reconciliation. The spreadsheet submission for (month day), 202(X) is a total of $(amount) in payments of the 27.5% portion of their health insurance. Fund R6163HTC."
-
For participants, the spreadsheet is submitted using:
Vendor number 02020069
Fund R6163HTC
-
-
Once the SF-1034 reimbursement spreadsheet for individuals has been submitted to CFO, it will be provided to the Enrollment team for batching, correspondence, and comments. P&A will send an email confirmation, to HQonce correspondence is issued.
-
For vendors, the disbursement process is completed by HQ and Standard Forms 1034 are submitted to CFO.
-
The 1034 reimbursements/disbursements will be added to the payment history within the HCTC database by P&A.
-
If the Enrollment Team is contacted regarding a reconciliation issue, elevate to P&A.
-
Use the following information, to complete SF-1034 for vendor disbursement.
-
Input the voucher number in the format of HPA/TPA MM-YYYY (M=month Y= year). For example, BCBSM 01-2017.
-
U.S. DEPARTMENT, BUREAU, OR ESTABLISHMENT AND LOCATION – HCTC Program Office
-
DATE VOUCHER PREPARED – Enter date voucher is prepared
-
CONTRACT NUMBER AND DATE, REQUISITION NUMBER AND DATE, SCHEDULE NO, and PAID BY– Leave Blank
-
DATE INVOICE RECEIVED – Enter date voucher is prepared
-
DISCOUNT TERMS – Leave Blank
-
PAYEE’S ACCOUNT NUMBER – Enter the vendor’s employer identification number (EIN)/taxpayer identification number (TIN)
-
PAYEE’S NAME AND ADDRESS – Enter the vendor identification number followed by vendor’s name and address. For example:
Vendor Number 00012345
John Doe Insurance
123 Main Street.
Anytown, TX 78704 -
SHIPPED FROM, TO, WEIGHT, GOVERNMENT B/L/ NUMBER, NUMBER AND DATE OF ORDER (column), and DATE OF DELIVERY OR SERVICE (column) – Leave Blank
-
ARTICLES OR SERVICES (column) – Enter a description for the reimbursement, the date of the return of funds (if available), the program name (HCTC AMP (Advance Monthly Payment)), and a breakdown of the government’s percentages and the participant’s percentage. For example:
Payment to (vendor) to reconcile (month(s)).
Return of Funds from (vendor) on (date)
HCTC AMP
27.5% portion = (calculate 27.5% of total)
72.5% portion = (calculate 72.5% of total) -
QUANTITY (column) and UNIT PRICE (column) – Leave Blank
-
AMOUNT – Enter amount of reimbursement
-
TOTAL – Enter total amount of reimbursement. This amount must match the APPROVED FOR amount.
-
PAYMENT (check boxes) – Leave Blank
-
APPROVED FOR – Enter the amount of reimbursement. This amount must match the TOTAL amount.
-
EXCHANGE RATE, DIFFERENCES, BY(2), and TITLE– Leave Blank
-
-
ACCOUNTING CLASSIFICATION Section
-
Enter the appropriate Accounting Classification Codes provided by CFO for the 72.5% appropriation account.
Fund: R0923HTC
Commitment: 41
Funds Center RA04
Functional Area - RMAD
Order - CHTC
Business Area – 0002 -
Enter the appropriate Accounting Classification Codes provided by CFO for the 27.5% appropriation account.
Fund: R6163HTC
Commitment: 2400
Funds Center RA04
Functional Area - RMAD
Order - CHTC
Business Area – 0002
-
-
Any documentation related to Form 8885, Health Coverage Tax Credit, received in the Entity unit should first be reviewed to determine if it is related to the Advanced Monthly Program or Form 1040.
-
If the documentation was sent in support of the Advanced Monthly Program, it should be processed following standard HCTC procedures.
-
If the documentation was sent in support of Form 1040, route to CIS/AM.
- Edit "(HCTC)" in the left margin
- Place in your route-out folder
-
-
Health Plan Administrators (HPA) and Third Party Administrators (TPA) must be able to receive payments via Electronic Funds Transfer (EFT) processed through the Direct Deposit Program as an Automated Clearing House (ACH) payment.
-
HPAs/TPAs must be enrolled in the EFT program to receive insurance premium payments for their customers who are participants in the HCTC program. Receiving electronic payments ensures timely, accurate payments and reduces the risk of payments being misdirected within the HPA/TPA’s organization.
-
HPAs and TPAs must complete Form 3881-A, ACH Vendor / Miscellaneous Payment Enrollment – HCTC, to enroll and begin receiving HCTC payments. If a vendor is not set-up as an approved HCTC vendor, correspond with Letter 4540 using selectable paragraph 12. See IRM 3.11.29.13.4, Letter 4540, HCTC Candidate Eligibility Denial.
-
Once a HPA/TPA has sent Form 3881-A and is established to receive payments, they do NOT need to submit another Form 3881-A if additional individuals enroll after the HPA/TPA is established.
-
However, a HPA/TPA must recertify each year by submitting a new Form 3881-A. See IRM 3.11.29.20.2, Recertifying with Form 3881-A, ACH Vendor / Miscellaneous Payment Enrollment – HCTC.
-
Form 3881-A, ACH Vendor / Miscellaneous Payment Enrollment – HCTC, is processed by the HCTC Headquarters Analyst. If attached to an application, elevate to the Coordinator.
-
Form 3881-A may be received through the Stakeholder mailbox, submitted with an application, or sent through the mail. If a physical form is sent in, scan the form and e-mail it to wi.hctc.stakehldr.en@irs.gov.
-
Health Plan Administrators (HPA) and Third Party Administrators (TPA) must recertify annually to receive insurance payments from their participants via Electronic Funds Transfer (EFT) through the Direct Deposit Program as an Automated Clearing House (ACH) payment by submitting a new Form 3881-A.
-
For Recertification:
-
HQ Analysts will provide a one-month notification to P&A either through e-mail or spreadsheet of upcoming renewals.
-
P&A will issue notifications as Forms 4442, Inquiry Referral , to the Enrollment Team. See IRM 3.11.29.14, Form 4442, Inquiry Referral.
-
The Enrollment Team will generate a Letter 5974, Annual HCTC Vendor Renewal Certification, for the HPA/TPA. See IRM 3.11.29.13.8, Letter 5974
-
The Enrollment Team will batch the notifications as Forms 4442. See IRM 3.11.29.14.
-
The Enrollment Team will notify P&A of completion and HQ will monitor the renewals.
-
-
HCTC participants are instructed to send their payments to a lockbox depository for payment processing.
-
If payment(s) received at the lockbox require additional information to process, such as a missing or invalid Participant Identification Number, Lockbox will request the missing information from the Enrollment Team, via email by 12:00 p.m. CST daily.
-
The Enrollment Team will research the HCTC database for missing information/invalid Participant Identification Number and provide a response to Lockbox by 10:00 a.m. CST the next business day ≡ ≡ ≡≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡.
-
If the Enrollment Team supplies sufficient information for the missing/invalid PIN, the Lockbox site will process the remittance.
-
If a valid PIN number cannot be located, Lockbox will reject the payment back to the participant with all original contents.
-
The Lockbox site will return rejected payments/unprocessable items back to the participant, with a reject letter. A copy of the reject letter and all contents that were mailed to the participant will be sent from Lockbox to the Enrollment Team, with a Form 3210, Document Transmittal, as part of a daily mail out package.
-
As part of the daily package mail-out to the Enrollment Team, Lockbox will include correspondence items and envelopes received at the Lockbox site in which the site processed the participant’s remittance. Correspondence includes an item received that is not a payment coupon or remittance.
-
The Lockbox site must use an approved dedicated overnight private delivery/ freight service (e.g., FedEx, DHL, and UPS) to deliver shipments to the Enrollment Team.
-
Once the shipment is received, the Enrollment Team will:
-
Verify the contents were received and sign the acknowledgment copy of the Form 3210. The Enrollment team will return the signed, dated and acknowledged Form 3210, to the Lockbox site by 2:00 p.m. local time, ≡ ≡ ≡ ≡ ≡≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡ ≡.
-
Batch the content as Form 4442s. See IRM 3.11.29.14, Form 4442, Inquiry Referral.
-
-
If Lockbox does not have a daily mail out package to send to the Enrollment Team, they will send an e-mail to the Stakeholder mailbox to advise there is no mail out package.
-
CFO will send an e-mail to the Stakeholder mailbox when insurance premium payments have been returned due to insufficient funds.
-
Insufficient Funds are worked by HQ.
-
The Rejected payments are worked by HQ.
-
CFO will send notification of rejected payments to the stakeholder inbox.
-
Once official notification of rejected payments is received, the payments are added to the Return of Funds (ROF) spreadsheet and tracked for the 27.5% reimbursement allowed on Standard Form 1034, Public Voucher for Purchases and Services other than Personal. See IRM 3.11.29.18, SF-1034, Public Voucher for Purchases and Services other than Personal, Monthly Payment Reconciliation.
-
Once payments are researched to determine both the cause of the return and where the payment should now be applied, they are added to the database by P&A and comments are added or updated in the database.
-
Operations Assistance Request (OARs) from Taxpayer Advocate Services are normally received through the Stakeholder mailbox (*W&I HCTC STAKEHOLDER ENGAGEMENT <WI.HCTC.Stakehldr.En@irs.gov>) and are worked by P&A.
-
If any OARs are received outside of the Stakeholder mailbox, refer to the HCTC Coordinator to be elevated to P&A.
-
Forms 13441-A, Health Coverage Tax Credit (HCTC) Monthly Registration and Update, must be retained in AUSP Files or designated area for six (6) years, then retired to the Federal Record Center (FRC) to follow the Record Retention requirements for Document 12990, Records and Information Management Records Control Schedules.
-
The Lockbox site must capture an image of the front and back of all remittances and the payment posting documents (vouchers, facsimiles, remittance photocopies) for all transactions they process.
-
The Lockbox site must retain electronically processed remittances for a period of five (5) business days after the electronic check processing (ECP) settlement date. These documents must be kept in a manner that is easily retrievable.
-
The Lockbox site must retain paper vouchers or payment posting documents/ facsimiles/photocopies for a period of five (5) business days after the ECP settlement date. These documents must be kept in a manner that is easily retrievable.
-
RTR (Image) files must be retrievable for a period of 30 calendar days from creation.
-
-
The following daily reports are prepared and submitted by Lockbox through the Stakeholder mailbox.
-
Daily Deposit Production Report
-
Payment Reject Letter Tracking Report
-
-
The Daily Deposit Production Report shows payments processed and other activity, such as overpayments.
-
The Payment Reject Letter Tracking Report must include the following:
-
The date the reject letter was mailed to the participant by Lockbox
-
Participant’s last name
-
Participant Identification Number (PIN)
-
A reason the item was rejected (A-H)
-
A daily count of the rejected items
-
-
If the reject reason is "H" (other), a comment must be added to explain the reason the payment was rejected. If payment was rejected for an invalid or missing PIN (Reason Code D) and faxed to the Austin Enrollment Team, the date and time of fax is entered.
-
The Lockbox Site must retain copies of rejected items such as reject letters, original payment coupons, remittances and correspondence on site for one year in retrievable format to support responses to government inquiries.
-
There are three weekly reports for the HCTC program: Weekly Statistical Report, HCTC Production Report, and the HCTC Weekly Refund Report.
-
Weekly Statistical Report. The report is received every Monday morning from the HCTC Coordinator or Entity Team Work Leader to provide weekly data on HCTC volumes.
-
HCTC Production Report. This report is received from P&A each Monday.
-
HCTC Weekly Refund Report. This report is received weekly from IRS Beckley Office and is used by HQ and P&A to reconcile payments. The report shows return of funds from Health Plan Administrators (HPAs)/ Third Party Administrators (TPAs). It is received with a zero balance if there are no return of funds for the week.

Please click here for the text description of the image.

Please click here for the text description of the image.

Please click here for the text description of the image.

Please click here for the text description of the image.
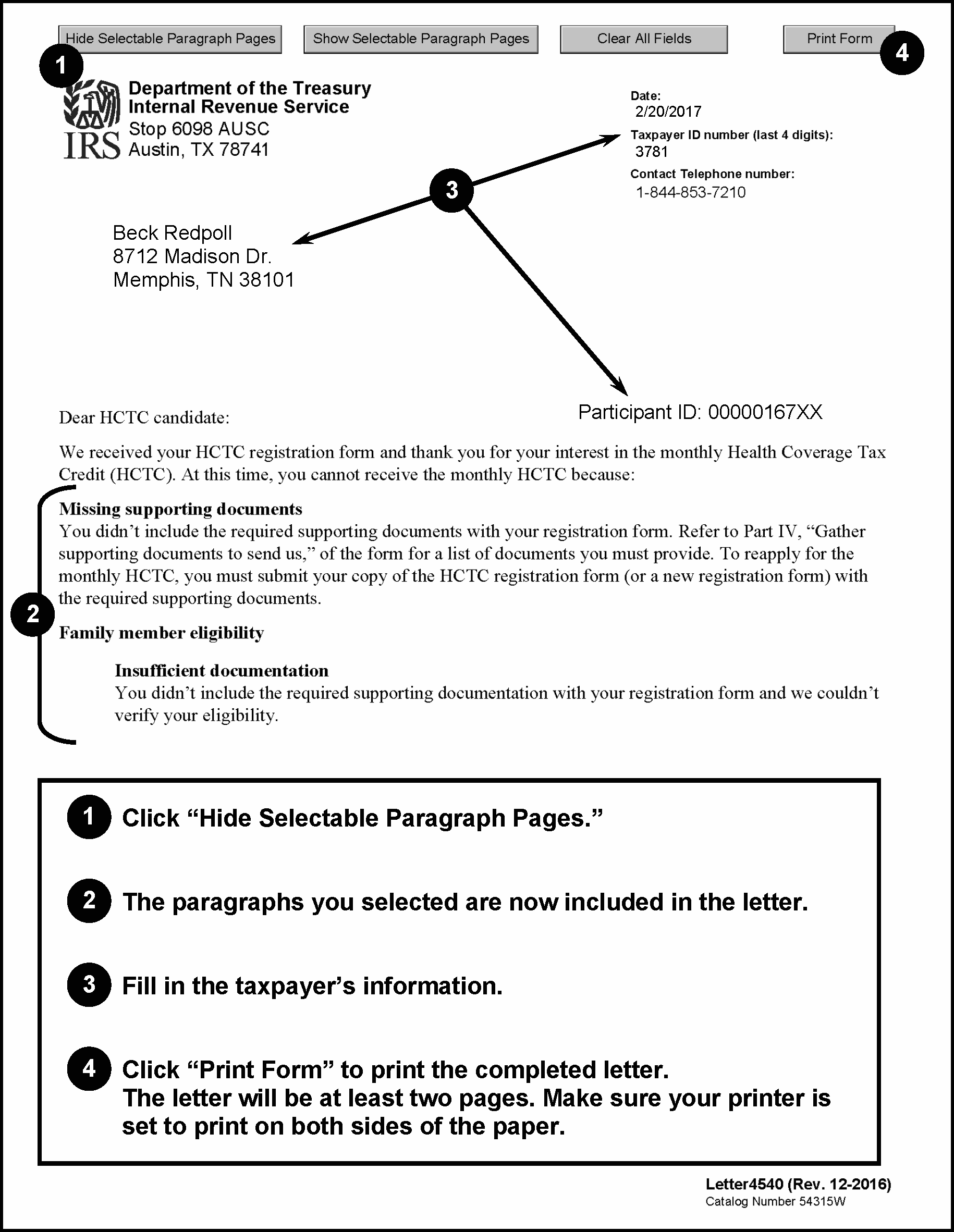
Please click here for the text description of the image.






 )
or https:// means you've safely connected to the .gov website. Share sensitive information only on official, secure websites.
)
or https:// means you've safely connected to the .gov website. Share sensitive information only on official, secure websites.